How Do Vaccines Work?
WHAT ARE VACCINES AND HOW DO THEY WORK? - Visual Description Transcript
[Animated George Washington writes a letter in his battlefield tent.]
[SHOTS FIRED, HORSES WHINNY]
[QUILL PEN SCRATCHING ON PAPER]
GEORGE WASHINGTON: The General has nothing more at heart than the health of the troops…
[Washington’s hand writes “Headquarters New York, 1776.”]
NARRATOR: In the early years of the American Revolution, the Continental Army had more to fight than enemy soldiers.
[Colonial soldiers take aim at oversized smallpox virus virions.]
NARRATOR: Smallpox was raging through the colonies—in some places killing up to half of the white settlers who fell sick,
[A group of silhouettes represent white colonists. Half of the figures darken to indicate the death toll.]
NARRATOR: …and taking an even deadlier toll on Native Americans, some of whom had been deliberately infected as a weapon of occupation.
[Silhouettes representing a small group of Native Americans darken, representing the disease’s devastation. Only a lone figure remains unaffected.]
NARRATOR: The British redcoats weren’t too bothered--the majority had already survived the disease as children— but American-born soldiers were at great risk.
[Smallpox virions bounce off a red military coat, representing the British soldiers, but swarm a blue coat, representing the American colonial forces.]
NARRATOR: George Washington, who’d had smallpox himself as a teenager, knew that many people were reluctant to be inoculated, or protected by receiving a less-deadly form of the virus.
[A cartoon version of the well-known Gilbert Stuart portrait of George Washington is surrounded by a group of colonial men wearing wigs. Washington’s wig is animated with smallpox particles, while those of the colonial men contain question marks.]
NARRATOR: But facing devastating losses, Washington wrote to Congress that he had determined to inoculate all the troops and new recruits.
[Scene transitions back to Washington writing a note in his battlefield tent. The note reads, “1777, The Troops Shall Be Inoculated.”]
NARRATOR: This decision undoubtedly saved lives and was probably a big part of why they won the war.
[OPENING NOTES OF THE AMERICAN NATIONAL ANTHEM]
[A cartoon version of the famous painting of Washington Crossing the Delaware River, but in this case, the boat is steered over smallpox virions instead of ice floes.]
NARRATOR: Vaccines are one of humanity’s greatest triumphs, and their development arose from knowledge across the globe. People have been using antiviral technology for centuries.
[The word “VACCINE” orbits around Earth, creating a shield. Cartoon virus particles bounce off the rotating globe.]
[In one hand, a woman holds a rag dripping with a fluid labeled “infectious pus.” With her other hand, she rubs the fluid into the arm of a patient.]
NARRATOR: The type of inoculation they used in the Revolutionary War—rubbing infected pus onto a healthy person to give them a milder case—originated hundreds of years ago in Asia and Africa.
[A map shows Africa and Asia, pulsing with red blobs.]
NARRATOR: Lady Mary Wortley Montagu brought it from Turkey to Europe. An enslaved Black man named Onesimus introduced it from West Africa to North America.
[A world map illustrates the path of knowledge from the Middle East to Europe, and from West Africa to North America. As the knowledge spreads, the red blobs give way to a solid, light purple color.]
[The scene transitions to a large cartoon syringe. Three cows float inside its empty chamber.]
NARRATOR: In the late 18th century, Edward Jenner discovered that patients exposed to cowpox were then protected from smallpox.
[The syringe’s plunger presses in, pushing out the cows and pulling in the word “VACCINATION.”]
NARRATOR: He called the procedure “vaccination,” after the Latin word for cow.
[The camera pans across the large syringe. A cow stands on the needle and onscreen text reads “VACCA = COW.”]
[COW MOOS]
[The camera tracks along with an animated vaccine plunger. Instead of lines indicating the level of dosage on the syringe, hashmarks are tagged with timeline years, from 1900-2000.]
NARRATOR: By 1900, we had vaccines against cholera, rabies, typhoid, and plague. And over the next hundred years, things really started to snowball.
[As the plunger moves along the syringe, names of diseases for which humanity developed vaccines pop up in its wake.]
NARRATOR: Vaccines offer incredible protection against formerly deadly diseases and vaccination now saves more lives than any other medical procedure.
[A variety of vaccine posters from all over the world scroll by.]
NARRATOR: But, how do vaccines work? Let’s look at what they’re trying to do in the first place.
[A large, animated syringe ejects fluid that draws out the word “VACCINE” before dropping down into a bowl.]
NARRATOR: Our natural immune system is pretty incredible. Think of it like a chef with lots of recipes.
[The camera reveals a wider shot of the bowl being stirred by a chef in a kitchen. On the counter is a cookbook titled “Cooking With Vaccines.”]
NARRATOR: It can cook up resistance to a whole slew of diseases. Vaccines, then, are like cookbooks--instructions that teach our chefs great new recipes.
[Two cans are labeled “DEAD VIRUS,” and “WEAKENED VIRUS.”]
NARRATOR: Most vaccines use either a weakened or dead form of a virus, or a harmless piece of its shell, to excite our immune system. They deliver the “ingredients” for immunity to our bodies, and using those ingredients, our immune systems whip up a recipe to protect us from a virus.
[The chef pours cans of “Weakened Virus” and “Dead Virus” into her mixing bowl.]
NARRATOR: So, if we ever meet that virus down the road, our immune system remembers how to get rid of it.
[The chef now stands behind a short order restaurant window. A ticket showing a virus is placed in the window. The chef serves up the bowl.]
[DING, A SERVICE BELL RINGS]
NARRATOR: For decades, researchers have been working on another type of vaccine—a messenger RNA, or mRNA, vaccine.
[A researcher holds a syringe. Text reads, “messenger RNA (mRNA).”]
[Scene transitions to a strand of mRNA floating by on the screen. The mRNA is an undulating single helix.]
NARRATOR: mRNA is already inside all of us. Its job is to relay instructions for making proteins--molecules that do all kinds of work in our bodies,
[A segment of mRNA animates up to look like a signpost. Arms branch out.]
NARRATOR: …like keeping our cells together,
[Text appears on the top branch of the signpost, reading “PROVIDE STRUCTURE.”]
NARRATOR: …helping our muscles move,
[Text appears on the second branch of the signpost, reading “MOVE MUSCLES.”
NARRATOR: …and protecting us from viruses.
[Text appears on the bottom branch of the signpost, reading “PROTECT AGAINST INFECTION.”]
NARRATOR: An mRNA vaccine delivers really specific and efficient instructions to our immune cells.
[Pages of a cookbook read, “Recipe with Ingredients,” and show a syringe with the word mRNA.]
NARRATOR: In the case of COVID-19, the mRNA tells our bodies how to make a spike protein from the shell of SARS-CoV-2, which causes COVID-19. Our immune cells cook up the recipe and, voila, produce a harmless, but recognizable spike.
[A chef stirs a bowl and reads a cookbook entitled “Spike Protein.” As she stirs, a spike protein like that on the surface of SARS-CoV-2 emerges from the bowl.]
NARRATOR: So, our immune system learns how to spot and destroy SARS-CoV-2 without ever being exposed to the actual virus.
[At the short order window, a ticket appears with a drawing of SARS-CoV-2. The chef pulls out the bowl with spike proteins.]
[DING, A SERVICE BELL RINGS]
NARRATOR: When the COVID-19 pandemic hit, we were able to develop mRNA vaccines so quickly because researchers have been working on the science behind them for more than 30 years.
[A drawing of a SARS-CoV-2 virion dissolves into a kaleidoscope of spike proteins, syringes, and the sweeping hands of a clock.]
NARRATOR: But a safe and successful vaccine takes more than scientists.
[Camera pans across scientists and syringes and lands on a patient being inoculated with a vaccine.]
NARRATOR: For a vaccine to be recognized as safe and efficient, it has to go through numerous tests. The three final phases are testing in volunteers--folks from all kinds of backgrounds. Each involves more people at every level and all new vaccines go through these trials—including the COVID-19 vaccines.
[Rows and rows of people rise up, one after another, all being vaccinated.]
NARRATOR: Scientists and medical professionals and volunteers from all over the world made this happen faster than ever before.
[A globe rises behind the many people being vaccinated.]
NARRATOR: But even as vaccination numbers climb in the COVID-19 pandemic, there’s more work to be done.
[Plungers depress on a row of syringes, and their contents form a rising graph line, representing more and more people being vaccinated. The camera pulls out to reveal even more syringes that still contain vaccine and a steep, dotted line, illustrating how much further we have to go before the world is vaccinated.]
NARRATOR: People must have access to vaccines and the education to move from hesitance to confidence. It’s within our power to end this pandemic, and vaccines will get us there.
[Animated versions of SARS-CoV-2 virions slither among a crowd of silhouettes. First one silhouette changes from dark into a golden glow, and then the glow spreads to all the people in the crowd.]
[Credits roll.]
Vaccine Questions in the Age of COVID-19
Vaccines have changed the course of human history. Over the last 200 years, they have reduced, eliminated, and, in the case of smallpox, even eradicated diseases that had plagued people for centuries.
So when a fast-spreading and dangerous disease—COVID-19—emerged, scientists worked at unprecedented speed to develop this line of defense against the new threat, too. COVID-19 vaccines drew on decades of research and new technologies, but most of these weren’t familiar to the public.
Even though billions of people have been vaccinated worldwide, others still have questions—some new to the COVID-19 pandemic, and some as old as vaccines themselves.
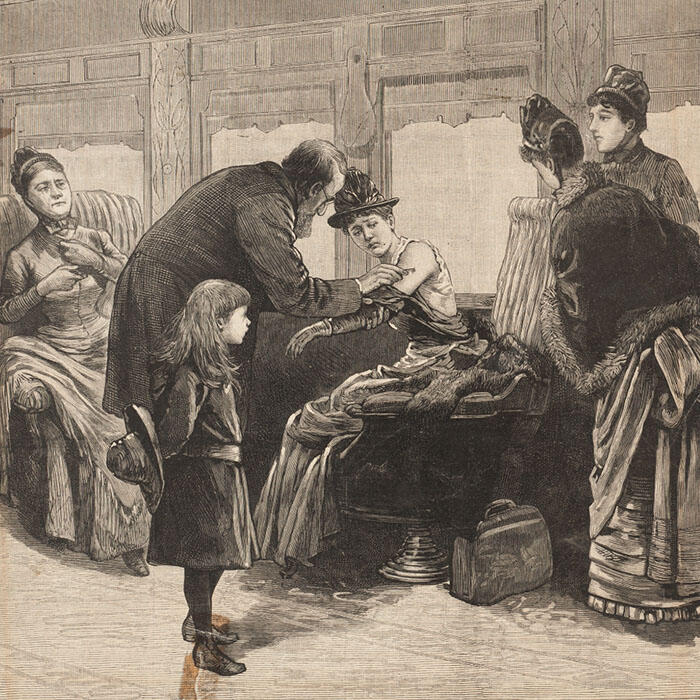 Vaccinating American-bound passengers on the Grand Trunk Railway of Canada during the Montreal smallpox epidemic of 1885.
Vaccinating American-bound passengers on the Grand Trunk Railway of Canada during the Montreal smallpox epidemic of 1885.Courtesy of J. Marvin/Osler Library of the History of Medicine, McGill University
 Drive-through vaccinations for COVID-19, April 2021.
Drive-through vaccinations for COVID-19, April 2021.Courtesy of M. Corvello/Wikimedia Commons
This is the most basic question—people want to understand whether a vaccine will protect them against a virus.
In the U.S., before a vaccine can be given, it has to go through carefully constructed clinical trials. One group of people is given the actual vaccine, another is given a placebo—a shot of a neutral substance such as salt water, for example—and neither the scientists nor the subjects know who is getting which. Then, after some time has gone by, the groups are compared to see whether there are differences in their rates or severity of infection or illness. All U.S. COVID-19 vaccines went through rigorous clinical trials, and all have been shown to lower risk of infection and severe illness due to COVID-19.
To judge how well a vaccine is working, scientists running a clinical trial measure how well it reduces risk of infection or illness compared to people who are not vaccinated. For example, let’s say 200 people participate in a trial, with 100 receiving the vaccine while the second half receives a placebo. If 50 people from the placebo group become infected and only 10 from the vaccinated group, that would mean the vaccine lowered the risk of disease by 80 percent. All COVID-19 vaccines authorized in the U.S. were tested with tens of thousands of trial participants. All were shown to be highly effective at preventing hospitalization and death due to COVID-19.
Experts want to understand both a vaccine’s efficacy (how well a vaccine does in clinical trials) and its effectiveness (how well it does in the real world). As new variants, such as Delta and Omicron, arise, the COVID-19 vaccines’ effectiveness is being constantly monitored.
But even vaccines with lower effectiveness can save lives and prevent widespread infection. For example, flu vaccines, which change from year to year to target different strains of the influenza virus, have an average effectiveness of 40 percent. Even so, they prevent millions of influenza cases and thousands of deaths each year in the U.S.
Ever since the 18th century, when William Jenner coined the term ‘vaccine’ and developed the first one to protect against smallpox, people have worried that side effects from vaccination could be worse than the disease. This is the leading cause of vaccine hesitancy.
Public health experts have been grappling with this concern ever since. It’s hard to convince healthy people to protect their health by taking an action that carries potential risk, even when not taking that action carries a far greater risk.
Decades of research and tried-and-true testing techniques are behind all vaccines, including the new ones. Doctors, nurses, and other health care providers can be trusted sources to speak with when we have questions about side effects.
DR. JENNIFER NUZZO, Associate Professor, Johns Hopkins Bloomberg School of Public Health: When you get vaccinated, your muscle cells take up the vaccine.
In the case of mRNA vaccines, your muscle cells take up messenger RNA that your muscle cells use to make the spike protein, which is the protein that the virus that causes COVID-19 uses to enter your cells.
Your cells make that spike protein so that your immune system can see it and be trained to recognize it.
The vaccine though doesn't circulate around your body. It's just taken up by your muscle cells.
The muscle cells use the mRNA, they make the spike protein. Your immune system goes after it. And then after a few weeks, it's gone. Gone from your body entirely.
No more spike protein, no more vaccine, gone.
What's left behind though is the knowledge of what that spike protein looks like, and your immune system uses that knowledge to respond if it ever sees the virus trying to enter your body.
[MUSIC PLAYING]
It’s important to acknowledge that just as medications can have side effects, so can vaccines. That’s why monitoring for side effects is a part of any clinical trial and continues once the vaccine is in use. It’s also important to understand the enormous risks that vaccine-preventable diseases present.
The benefits of getting a vaccine are much greater than the possible complications—both short- and long-term—from a disease like COVID-19. For example, myocarditis, or the inflammation of the heart muscle, is a very rare side effect of the COVID-19 vaccine that has been documented among mostly male teens and young adults. But the risk of the same condition after infection with COVID-19 itself is several times higher.
“The myocarditis that occurred with the vaccine is mild compared with what we know as virus-associated myocarditis,” says Sallie Permar, chair of the Department of Pediatrics at Weill Cornell Medicine in New York City, who notes that in her experience, COVID 19-associated myocarditis requires longer hospitalization and even life-saving interventions. In most cases of myocarditis after vaccination, patients recovered fully with treatment and rest.
Questions about how vaccines may affect existing health problems are common.
When people are burdened by underlying conditions and have less access to high quality care—as is the case for those who continue to face medical racism and health care inequities, including Black, Latino, Native American, and many immigrant communities—these questions and concerns may be harder to address and resolve.
Underlying conditions put us at increased risk for severe illnesses, including COVID-19. So, vaccine trials are designed, in part, to test whether vaccines are safe and effective for people with different conditions. Trials of all three COVID-19 vaccines available in the U.S. included thousands of people with common health problems: at least 20 percent of participants in the final phases of testing had high blood pressure, diabetes, chronic pulmonary disease, HIV, or obesity. The trials’ developers recognized the importance of having volunteers that reflect the diversity of our population, and the trials showed that the vaccines were safe and effective in people with underlying conditions.
In addition to encouraging vaccination, public health experts stress that we must also address longstanding inequities, rooted in racism and economic disparity, that prevent people from accessing the resources they need for their health and wellbeing. “We really need to work on some long-standing issues,” says Johns Hopkins University Professor of Equity in Health and Healthcare Lisa Cooper. “Things like access to safe housing, to water, to food, to a job that pays a living wage, and to healthcare…That way, people will be as healthy as they can possibly be, and they’ll be in the best position to protect themselves when there’s a crisis like a pandemic.”
There is a history of harmful and unethical behavior by governments and corporations that carried out policies without the wellbeing of all people in mind. For example, the infamous Tuskegee study, which was run by the U.S. government from 1932 to 1972, withheld syphilis treatment from infected Black men for decades, and some participants even died as a result. And at the turn of the 20th century, compulsory smallpox vaccination was at times carried out through nighttime police raids in poor, immigrant, and Black communities.
Distrust has not been limited to harmed and marginalized communities. During Boston’s last smallpox outbreak, in the early 1900s, politically powerful white communities resisted compulsory vaccination as government overreach and a violation of individual liberties.
Today, sharp political divisions exacerbate distrust of government and medical experts. Building trust and confidence requires transparency and working with community partners to provide education about COVID-19 and access to vaccines. In New York City, the Department of Health partners with dozens of groups across all boroughs.
Health outreach through trusted community partners has been shown to work—for example, in one study, Black barbers encouraged Black patrons to meet with specially trained pharmacists at their barbershops to receive blood-pressure medication. The patrons reduced their blood pressure and successfully kept it down.
Different disease-causing viruses induce different immune responses. For some diseases, an infected person will gain lifelong immunity. But for other illnesses, such as COVID-19 and influenza, people can be infected more than once, leaving them vulnerable to the disease and its complications.
Vaccines for COVID-19 have been shown to help lower the risk of re-infection for those who have had the disease —something that’s especially important in places and during periods when community infection rates are high and when new and dangerous variants are circulating. Studies have also shown that people respond differently to COVID-19 infection; some don’t develop immunity after they recover. Getting a vaccine—even after being infected with COVID-19—reduces the risk of reinfection.
Furthermore, getting vaccinated isn’t just for individual safety. Vaccinated people limit transmission and infection for everyone. We need to understand the benefits vaccination conveys to our friends, family, and other community members who may be more vulnerable. We’re all in this together!
More to Explore
Created with the support of the City of New York Department of Health and Mental Hygiene. © 2023 City of New York